A Question
Tendon problems include traumatic injuries such as rupture, rapidly worsening problems such as tendonitis (inflammation) and slow developing chronic problems such as tendinosis (non-inflammatory tendon breakdown)[1]. These later two are often blamed on overuse and poor bio-mechanics.
But you might be asking “Why is my achilles sore when that other guy with terrible running form is doing twice the mileage as me?” or “why do I have posterior tibial tendon dysfunction when Haile Gebreselassie ran with a ridiculous amount of overpronation and and I’ve never heard of problems with his tibialis posterior or achilles tendons [2,3]?
As a doctor of physical therapy, I face these “why me” questions frequently and lucky for you, I have read the available research literature to bring you the best answer.
Some Background
Tendon Function
Tendons are the elongated connective tissue attachments between muscle and bone. Long tendons in particular have two important functions:
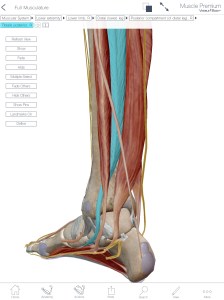
1) Allow muscles to be placed conveniently close to the center of the body. Because of its long tendon, the tibialis posterior in the calf can hold up the arch of the foot without bulking up the foot.
2) Help store elastic energy to produce explosive movements. The Achilles tendon is the largest and strongest tendon in the body and is estimated to sustain loads up to 12.5x body weight when running at 13.4mph [4]. Together the tendons and ligaments of the foot return an estimated 93% of the energy they absorb to the ground for propulsion [5], while stretching less than 4% [6].
The tibialis posterior tendon is highlighted in blue. Notice how the thin tendon loops around the arch of the foot and holds it up. Screenshot from Visible Body Muscle Premium for ipad
Tendon Composition
Tendons are made up of 60% type 1 collagen and varying degrees of type III, V, XIV and XVI collagen and supporting cells according to tendon’s function. The composition of the tendon of the supraspinatus in the rotator cuff and the patellar tendon aren’t exactly the same [7].
Tendon Turnover
Like all connective tissue in the body, tendons are constantly under renovation [8]. Enzymes such as matrix metalloproteinases break down collagen and tenocyctes make new collagen [8]. More loading stimulates the growth of more collagen, less loading and the tendon is broken down to the minimal level needed [8]. Tendon’s need this loading to be healthy, a week of bed rest and the tendon shrinks dramatically [4]. This process has helped us survive by 1) saving valuable protein and energy and 2) Removing an damaged tissue to keep the tendon functioning optimally. The take home messages are that 1) you don’t have the same tendon that you did, say 5 years ago, piece by piece the entire thing has been rebuild and 2) Your tendons need to be loaded to stay healthy.
At this point you are probably asking: If the tendon is constantly being renewed, how do we end up with tendon problems?
The Source of Tendon Problems
Disregarding the sword fights and wood shop accidents:
tendon injuries occur when the damage caused by loading the tendon is greater than the tendon can repair.
The formula is simple but the ways in which different factors in LOADING and REPAIR vary and interact with one another is complex. While most of the loading factors have the potential to be changed in some way, most of the repair factors don’t.
1) LOAD. They aren’t all easy to change but at least there is a chance.
- Training Error: Although the body has an incredible ability to adapt, it needs time to do so and can only handle so much of an increase at a time. People that go from being sedentary to highly active or that suddenly change the surface they run on are particularly prone to outpace the ability of their tendon to adapt. [9]
- Body Weight: A link between obesity, posterior tibial tendon dysfunction and flat feet has been found in the elderly [10]
- Bio-mechanical Faults: Fatigue, strength, flexibility, balance and simply the way you move effect how, and how much, your tendons are loaded. Two basketball players may complete the same number of layups, but the one with less ankle dorsiflexion will be more likely to get patellar tendinopathy [11]. The precise factors vary for each tendon but the good news is that they can often be changed with physical therapy.
2) REPAIR. This is the dark side of tendon problems and part of the answer to the most frustrating “why me” questions.
- Age: As tendons are constantly being rebuild, they aren’t rebuild quite as well each time. This is probably the result of accumulation of defects in the DNA, copying errors etc. Examination of achilles tendon from autopsies shoes degeneration beginning at age 35 [2].
- Genetics: Sex: Women have 3x higher risk of posterior tibialis tendon dysfunction [12] while men have higher risk of achilles tendonopathy [2].. It isn’t clear how much of this is due to different behavior, biomechanics, or tendon cell function.
- Genetics Body Structure: Factors found to have some association with posterior tibial tendon dysfunction: Uneven leg length, a shallow groove in the medial malleolus for the tendon, an accessory navicular bone.
- Genetics: Tendon Biology: Different gene variants have been found to correlate with pathology of different tendons but most of the variants involve the tendon breakdown enzymes or tendon building process. Here are a few examples
- TIMP2 inhibits the action of the collagen breakdown enzyme MMP. The rs4789932 variant of this gene was more common among the 178 subjects with tendinopathy than the 342 controls. Just the opposite was found for the GG variant of the ADAMTS14 gene which is part of the collagen forming process. [13]
- The BstUI ” restriction fragment length polymorphism” related to MMP-8 was more common among the 50 women who had breakdown of the tibialis posterior tendon for no apparent reason [14].
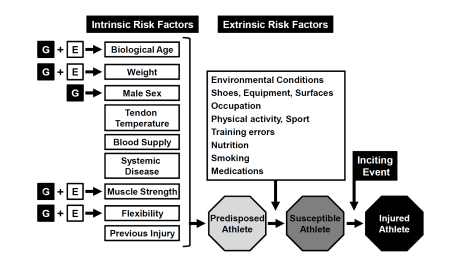
This model of the risk factors for achilles tendon injury highlights the complexity and includes several factors I didn’t mention. G stands for genetic and E for environments [15].
My Conclusion
The chance of getting a tendon problem is a combination of things you do and the luck of the draw. Although the factors I have described increase the risk of getting the problem, it is not clear how they influence the effectiveness of treatment. Treatment of tendinosis is for the most part effective, but current treatments such as eccentric exercise are time consuming to perform and improvement occurs gradually over the course of months. While many people who have genetic risk factors for tendon problems never get them, and many people with tendon problems don’t have the genetic risk factors, it remains to be seen whether the development of genetic specific treatment programs will speed the recovery process in the future.
References
- Maffulli N, Khan KM, Puddu G. Overuse tendon conditions: time
to change a confusing terminology. Arthroscopy 1998; 14: 840-3. - 2010 Achilles Tendinopathy Clinical Practice guidelines JOSPT. Cites several studies that linke speed and amount of pronation to achilles tendinopathy.
- Haile Gebreselassie’s pronation: https://www.youtube.com/watch?v=EAW87NsiGuI
- Jonsson P. Eccentric trianing in the treatment of tendinopathy. Dissertation Umea University Sweden. 2003.
- 2004 Tim Noakes “The Lore of Running” page 770 Citing: Alexander 1987, Ker et al 1987, and Alexander and Bennett 1989
- Sharma P, Maffulli N. Tendon injury and tendinopathy: healing and repair. J Bone Joint Surg Am.
2005;87:187-202. - Silver FH, Freeman, J. W., & Seehra, G. P. (2003). Collagen self-assembly and the
development of tendon mechanical properties. Journal of Biomechanics, 36(10), 1529–
1553. - Metabolic activity and collagen turnover in human tendon in response to physical activity
- Riley GP: The pathogenesis of tendinopathy: a molecular perspective. Rheumatology 43: 131, 2004.
- Kohls-Gatzoulis JA, Angel JC, Singh: Posterior tibial tendon dysfunction as a cause of flatfeet in elderly patients. The Foot 14: 207, 2004.
- 2011 Backman- Low range of ankle dorsiflexion predisposes for patellar tendinopathy in junior elite basketball players: a 1-year prospective study.
- Kohls-Gatzoulis JA, Woods B, Angel JC et al: The prevalence of symptomatic posterior tibialis tendon dysfunction in women over the age of 40 in England. Foot Ankle Surg 15: 75, 2009.
- 2013 Khoury- Polymorphic variation within the ADAMTS2, ADAMTS14, ADAMTS5, ADAM12 and TIMP2 genes and the risk of Achilles tendon pathology: a genetic association study.
- 2014 Godoy Santos- MMP-8 polymorphism is genetic marker to tendinopathy primary posterior tibial tendon.
- 2012 Raleigh- Gene variants that predispose to achilles tendon injuries an update